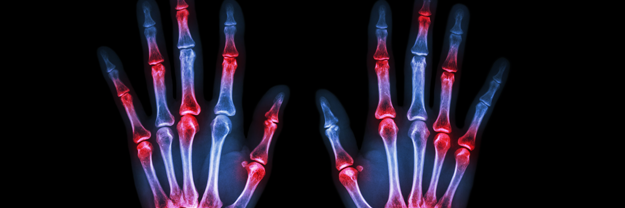
What does rheumatoid arthritis mean?
Rheumatoid arthritis (RA), as well as chronic polyarthritis, is the most common type of inflammatory joint diseases. It leads to pain, stiffness, swelling, and even loss of function of the affected joints. The incidence in the world-wide population is estimated at 0.5 to 1%. In Germany, about 800,000 people are affected, 70% of them women. The most common age for diagnosis is between 35 and 45 years old. However, the disease can already appear at a much younger age: 20,000 to 30,000 children in Germany under the age of 16 are suffering from a form of rheumatoid arthritis known as juvenile idiopathic arthritis.
The disease often manifests itself in small joints, such as those of the hands or the finger joints located closest to the hand. A typical characteristic is also the anatomically symmetrical spreading of the disease, meaning that, for example, most of the time both the left and right hand are affected. The course of the disease varies from patient to patient, it is possible that the disease is only temporary – up to 2 years – and then subsides without any further consequences. In contrast, a mild to moderate progression is characterized by the fact that the disease progresses in phases, alternating between phases with worsening symptoms – so called flares – and phases in which the symptoms fade – so called remissions. In the worst case there are no remissions, the disease persists for many years and leads to such violent joint damage that it can result in a severe disability of the patient.
The joint pains experienced daily by RA patients can lead to substantial cut-backs in their family, social, and professional lives.
Rheumatoid arthritis can also be expressed in other ways for certain people. For one quarter of the affected, rheumatic nodules are formed (little knots under the skin in proximity to the joint), others develop anemia, and it sometimes, though rarely, leads to neck pain, dry eyes, or a dry mouth.
What happens in the joints affected by RA?
The capsules of a healthy joint consist of an inner membrane, the synovium, which secretes the joint fluid. In the case of RA, misrouted immune cells enter the joint to the synovium and activate bone-degrading cells there. They also cause a typical inflammation (synovitis), symptoms including warmth, redness, swelling, and pain. A tumor-like tissue (pannus), which is ultimately responsible for the destruction of the functional structures of the joints over time, forms on the synovium. The other components of the musculoskeletal system, muscles, tendons and ligaments, which are connected to the joint, are likewise affected in their functions by the inflammatory response, resulting in the known pain and deformities.
How is rheumatoid arthritis diagnosed?
The initial diagnosis is difficult as there is no test that can give a definitive answer, but also because symptoms vary from patient to patient. Rheumatoid arthritis can also be easily confused with other joint diseases.
In order for a doctor to give a proper diagnosis, an informative conversation with the patient is essential. A physical examination can give clues as to how far along the disease is. Blood tests carried out in laboratories to determine relevant parameters for this disease provide further assistance in the diagnosis. Thus, most patients show to have a specific antibody, the so-called rheumatoid factor, in their blood. But this test too can not be adequately certain because there are both: RA patients without the rheumatoid factor and people that test positive to the rheumatoid factor, but never fall ill with RA. Furthermore, the number of leukocytes (the white blood cells) gets determined, as well as the erythrocyte sedimentation rate and the concentration of the C-reactive protein, whose elevated levels indicate an inflammatory response in the body. The blood also gets tested for anemia.
With an x-ray examination of the affected joints, the diagnosis can be ensured and the extent of the joint destruction that has already occured determined.
The causes of the disease:
As with so many diseases, the cause for rheumatoid arthritis is not fully known. Currently, it is sorted under autoimmune diseases, i.e. those diseases where the immune system attacks healthy cells in your body by mistake, in this case degrading the articular cartilage. A number of factors appear to contribute to the onset of the disease. What is certain, is that specific genes responsible for the characteristics of the immune system, are associated with the predisposition of RA. However, the presence of these genes does not necessarily lead to the outbreak of the disease. Rather, it is assumed that something else must occur to trigger RA, for example a viral or bacterial infection. In recent years, cytokines have been assigned a certain role in the onset of RA. Cytokines are substances formed by body cells that allow a kind of communication between cells and cell systems and also perform this function within the immune system. The cytokines responsible for triggering and amplifying the inflammatory response in RA are TNF-alpha and interleukin-1.
However, it should be noted that in general, the development of rheumatoid arthritis is caused by multiple factors.
How is rheumatoid arthritis treated?
The aim of the therapy is pain relief, inflammation inhibition, and the deceleration or even impedement of the progressive joint destruction. An improvement of the general condition and maintaining the operability of the affected joints are also desirable.
The earlier that RA is diagnosed, the better the treatment can work. The therapeutic window for optimal treatment success is very small: between 12 and 16 weeks after onset of the disease. Depending on the individual case of the patient, it is important to choose the most effective form of therapy for that patient, which can vary with how far the disease has progressed. Each therapy is always a combination of individual approaches, which include a change in lifestyle, any necessary surgeries, the regular medical monitoring with inspections and, most importantly, the medical treatment.
Medical treatment
The medical treatment for RA is continuously ongoing for most people. The available therapeutics can be sorted into four groups:
1) Acetylsalicylic acid and other nonsteroidal antiinflammatory drugs (NSAID)
Examples:
- pure and buffered acetylsalicylic acid
- ibuprofen
- naproxen
This group of substances aids to relieve pain and reduce inflammation and has traditionally been given at the start of the disease.
2) Glucocorticoids for inflammation inhibition
Examples:
- prednisone
- methylprednisolone
3) Biologics
In this case, biologics could be antibodies, soluble receptors, or antagonists. This latest, very expensive approach in RA therapy aims to trap endogenous inflammatory neurotransmitters and thus make them harmless.
Examples:
- adalimumab
- anakinra
4) Disease modifying anti-rheumatic drugs (DMARD): slow-acting antirheumatic drugs (LDAR) and disease-controlling drugs
These drugs combat the disease by intervening in the progression of the disease and modifying it on a long-term basis, hoping to bring it into remission. 97 % of all rheumatic patients receive a DMARD, underlining their importance in the treatment.
Examples:
- methotrexate
- hydroxychloroquine
- gold preparations
- penicillamine
- sulfasalazine
The different therapeutics work in different ways, therefore a combination of the available medications is used for treatments nowadays. For example, DMARDs can be combined well with a glucocorticoid or NSAID.
In the field of anti-inflammatory drugs, HEYL can look back on many years of experience – the first product of the company in 1926 was Polyphlogin®, a very common anti-rheumatic in its time. In 1955, HEYL succeeded in manufacturing D-penicillamine, being the first company in Germany to do so. Even today, D-Penicillamine is still used in special cases for the treatment of chronic polyarthritis. In the product roster of anti-inflammatory drugs, a generic sulfasalazine was introduced as another DMARD in 1993. Patients for whom methotrexate is contraindicated can be treated instead with sulfasalazine.
Additional information